Diabetes affect on your Oral Health

Diabetes affects oral health with Solutions
Diabetes, it might surprise you to know, is actually a symptom of a much more insidious disorder—insulin resistance. It refers to the body’s inability to use the insulin produced by the pancreas, either because it is deficient or insufficient. When insulin in the body is unable to open up cells and allow the intake of glucose, this glucose builds up in the bloodstream, leading to high blood sugar levels (BSL).
When this happens for an extended period of time, it leads to diabetes. The excess sugar in the blood travels to every part of the body and is thus the reason for the many complications—like deteriorating vision, nerve damage, heart issues, kidney problems, etc.—that we attribute to diabetes. One of the organs thus affected is the mouth.
When blood sugar is not controlled properly, high blood sugar weakens the white blood cells, which are the body’s primary defense against bacteria, and oral issues are quite likely to develop. However, research has consistently shown that when blood sugar levels are properly controlled—I.e. lowered to the recommended levels—the risk of damage to the body’s organs, such as the eye, heart, nerves, etc.—also drops. So, the first step in reducing the risk of dental problems for diabetics is to lower BSL.
Common oral health problems associated with diabetes
Some of the problems that diabetics are at risk from include: Dry mouth Sustained high blood sugar decreases the production of saliva, which results in a dry mouth. This is a prime condition for soreness, ulcers, and tooth decay.
Gingivitis and periodontitis (gum inflammation):
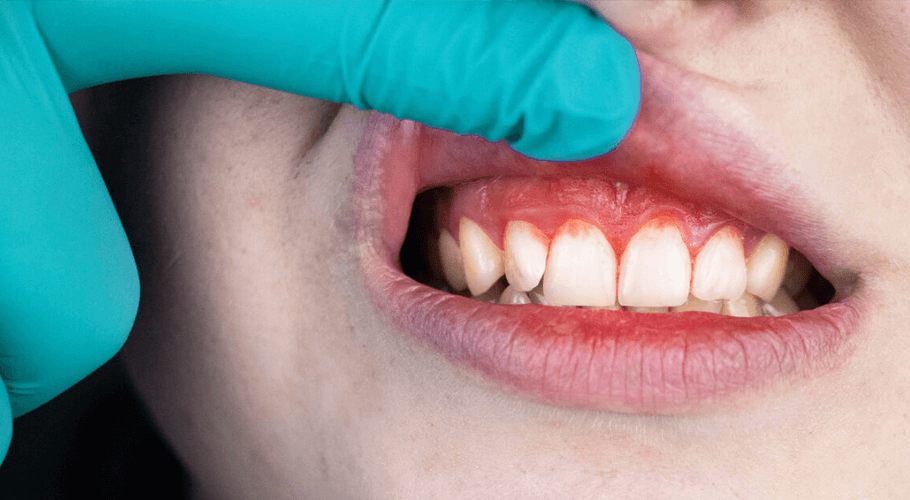
One of the effects of high blood sugar is a gradual thickening of the walls of blood vessels—which, if unchecked will lead to high BP. This slows movement of nutrients into the cells and the secretion of waste products from the various tissues of the body.
When combined with the damage to white blood cells and the reduced nutrient intake, the body begins to weaken and as bacteria grow, infections rise.
Periodontal diseases, it should be remembered—are caused by bacterial infection. Thus if diabetes is left unchecked, it will lead to recurring oral problems and more serious gum diseases.
Damaged healing capacity
As blood flow through the body decreases, the body’s ability to heal quickly is impacted. When this happens dental procedures, especially those that involve surgeries, begin to heal slowly.
Oral Thrush
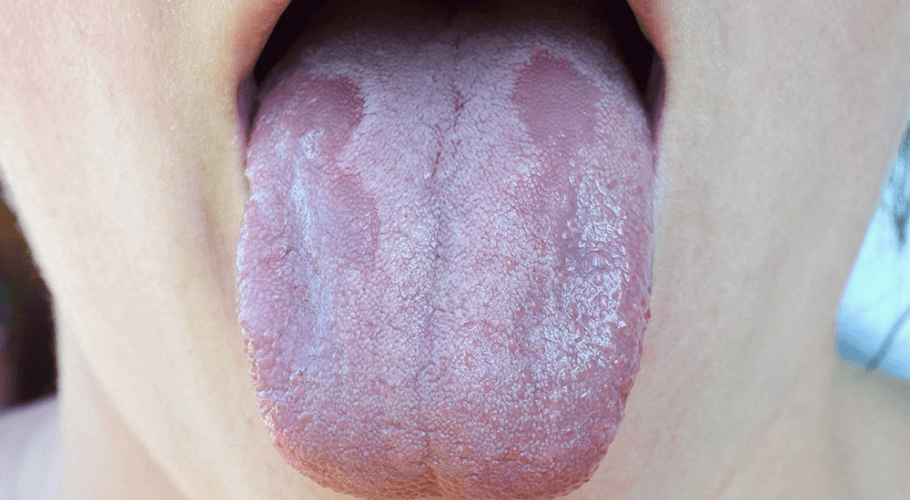
Because the body’s ability to attack infection is undermined, diabetics who may need to frequently take antibiotics to address infection, become prone to fungal infections of the mouth and tongue.
High glucose levels in the saliva help the fungus to thrive. Dentures—especially if worn constantly—can also lead to fungal infections.
Burning in the mouth or tongue
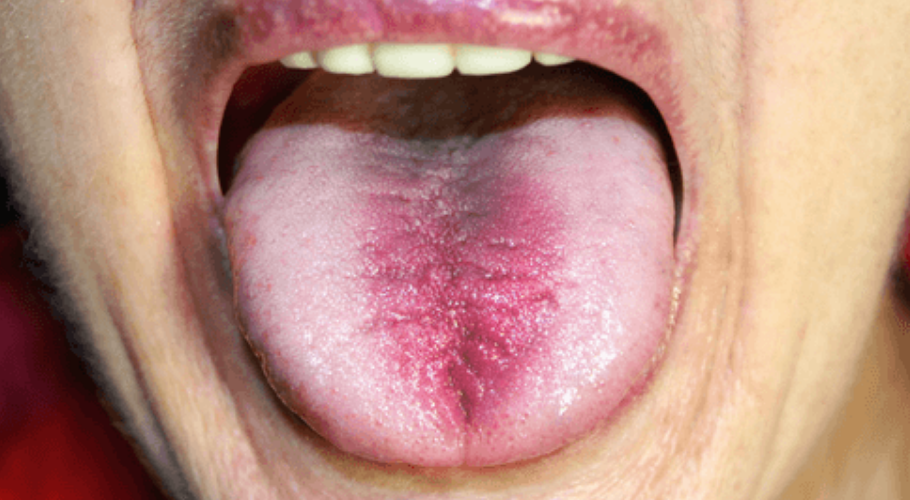
Thrush is responsible for this symptom. Smoking can also raise the risk of thrush; in fact, smokers are 20x more likely to contract thrush or periodontal disease, than nonsmokers.
Smoking also impairs blood flow to the gums, in turn negatively impacting the healing of wounds in this area.
Risk of dental cavities
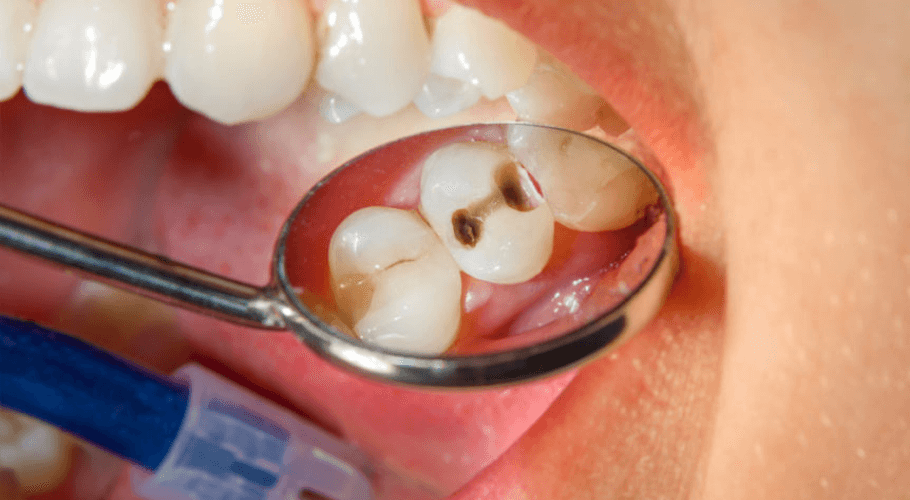
The high levels of glucose in the saliva of diabetics help bacteria grow, leading to tooth decay gum disease, and cavities.
Further, since diabetics tend to eat small but more frequent meals, it further increases the opportunity for bacteria to form and thrive.
Preventions:
If you suffer from diabetes, it is imperative to follow proper oral hygiene practices. If you notice any problem or change in your oral region, visit your dentist immediately. Some things you can do to reduce the chances of oral health problems include:
- Maintain recommended blood sugar levels
This means monitoring your BSL regularly. Take the HbA1C test every three months—it will tell you the average level of your blood sugar during the past three months. This reading should ideally be below 6.5%. - Be aware of the chances of hypoglycemia: (low blood sugar):
This is especially pertinent if you are on insulin. If you’ve already suffered an episode, tell your doctor. Inform your doctor of such episodes, frequency, and when you took your last insulin dose.
- Follow proper oral hygiene
Get your teeth and gums checked by a dentist regularly—your dentist will tell you how often you need to be checked. To prevent plaque from building up, brush twice and floss daily.If you wear dentures, ensure you take them out, clean them and air them daily
- Stop smoking
It’s a nasty habit and the dividends of stopping are immense.
In the event of dental surgery
If you need dental surgery, it is advisable to keep your dentist informed of your condition. If possible, get your doctor to talk to your dentist. They will inform you if you need to go on pre-surgery antibiotics, or if you need to adjust your medications and/or meals.
Ensure you inform your dentist of all the medicines and dosages you are taking. This is important, not least to ensure, your dentist doesn’t prescribe any medicine that could interact or interfere with your existing medications.
Finally, if your BSL is not ideal, and the surgery is elective, consider postponing the procedure. However, if you happen to be suffering from quick-developing infections, such as abscesses, get them treated urgently, as they can soon escalate.
Post-surgery, follow your dentist’s instructions religiously. Bear in mind that diabetics heal slower than non-diabetics.
Conclusion
There is evidence to show that people with uncontrolled diabetes are more susceptible to dental problems. They also tend to lose teeth more frequently than non-diabetics and are prone to gingivitis other dental infections—which don’t resolve quickly, precisely because of diabetes.
So it is critical for people with diabetes to pay close attention to their teeth. Practice good oral hygiene. Brush twice a day, at least; preferably after every meal.
Floss at least once a day. And modify your diet and exercise routines to keep your BSL under control. Doing all this will minimize the risk of infection and periodontal disease, as well as the possibility of tooth loss.
Combine self-care with medical attention (dental and diabetic) and keep your BSL as close as possible to ideal, and your risk from diabetes-related oral problems will be no greater than in non-diabetics.
Disclaimer:
This Blog solely serves our marketing purposes, for Authentic knowledge for this topic, Please Discover Reversal Session

