
Freedom from Diabetes
Research Foundation
Diabetes remission is defined as Hba1c < 6.5 without medications for at least 3 months. This possibility and arena of diabetes remission research is growing at a rapid and exciting pace as more and more diabetics seek deeper solutions across the world.
We at the Freedom from Diabetes Research Foundation are committed to identifying, implementing and publishing holistic and sustainable methods for reversing diabetes, its complications (related to eyes, heart, kidneys, nerves, etc) and related metabolic disorders (related to obesity, high cholesterol, hypertension, hypothyroid, PCOD, etc)
Scientific Publications
PUBLISHED RESEARCH
-
Insulin Resistance and Beta-Cell Function in the Context of Dyslipidemia in a Non-obese Indian Population with Type 2 Diabetes
Abstract:
Introduction
Insulin resistance (IR) and impaired beta-cell function (BCF) are central to type 2 diabetes (T2D) pathogenesis and influence lipid metabolism, causing dyslipidemia. While most dyslipidemia studies focus on obese individuals, data on non-obese populations are limited. This study explored the association between IR, BCF, and lipid profiles in non-obese Indian T2D patients.
Methods
A cross-sectional analysis was conducted on T2D patients (n=667) with a body mass index <25 kg/m², not on insulin or lipid-lowering medications, who participated in a one-year lifestyle intervention program at the Freedom from Diabetes Clinic, India. Clinical, anthropometric, and biochemical data were extracted from existing records. IR and BCF were assessed using homeostatic model assessment of IR (HOMA2-IR) and BCF (HOMA2-%B).
ResultsThe median age, HbA1c, and diabetes duration were 50 years, 7.6%, and nine years, respectively. Overall, 73.3% (n=489) were male, 4.2% (n=28) had IR (HOMA2-IR≥2.0), and 69.9% (n=466) had reduced BCF (HOMA2-%B<50). HOMA2-IR showed a positive correlation with triglycerides and non-high-density lipoprotein cholesterol (non-HDL-C) (P<0.001) and a negative correlation with HDL-C (P<0.001). HOMA2-%B was negatively associated with total cholesterol, low-density lipoprotein cholesterol (LDL-C), non-HDLC, and HDL-C (P<0.05). Receiver operating characteristic (ROC) analysis demonstrated that triglycerides (area under the curve (AUC)=0.648, P=0.008), non-HDL-C (AUC=0.626, P=0.023), and HDL-C in men (AUC=0.706, P=0.003) had fair discriminatory ability for IR. HOMA2-%B failed to discriminate lipid abnormalities.
Conclusion
In non-obese Indian T2D patients, both IR and beta-cell dysfunction are associated with dyslipidemia. However, only IR demonstrated a fair discriminatory ability for identifying abnormal lipid profiles, whereas BCF did not. These findings underscore the need for further studies to understand the metabolic drivers of lipid abnormalities in this population.
-
Type 2 diabetes remission and its predictors in an Indian cohort: A retrospective analysis of an intensive lifestyle intervention program
Abstract:
Predictors of type 2 diabetes (T2D) remission following intensive lifestyle intervention (ILI) are poorly characterized, especially in high-risk populations, such as India. This study aimed to identify the key predictors of T2D remission after an ILI in an Indian population. This retrospective analysis included 2384 patients with T2D (age 30–75 years; body mass index (BMI) ≥23 kg/m² enrolled in an online one-year ILI program at the Freedom from Diabetes Clinic, India, between May 2021 and August 2023. The intervention included personalized plant-based diet, physical activity, stress management, and medical support. Remission was defined as maintaining glycated hemoglobin (HbA1c) < 48 mmol/mol (6.5%) for ≥3 months without glucose-lowering medications. Anthropometric and biochemical data were extracted from clinical records. Predictors were assessed using logistic regression analysis. Post- intervention, 744 patients (31.2%) achieved remission The remission group showed significantly greater improvements in weight (−8.5% vs. −5.2%), BMI (−8.6% vs. −5.2%), HbA1c (−15.3% vs. −12.4%), fasting insulin (−26.6% vs. −11.4%), and homeostatic model assessment of insulin resistance (HOMA-IR) (−37.3% vs. −19.7%), than the non-remission group (p <0.05). The predictors of remission included age (≤50 years), higher BMI (≥25 kg/m²), drug-naïve status, shorter disease duration (≤6 years), juice fasting, baseline HbA1c <7%, weight loss >10%, and post-intervention HOMA-IR <2.5 (p <0.05). Our findings demonstrate that a significant proportion of individuals with T2D can achieve remission through a comprehensive culturally adapted lifestyle program. The identification of both baseline and post-intervention predictors underscores the importance of early, personalized, and holistic care in diabetes management.
-
Retrospective Analysis of the Efficacy of Integrated Lifestyle Modifications in Managing Prediabetes in the Indian Population
Abstract:
Background: Prediabetes is a growing health concern in India, with a prevalence of 15.3%. This retrospective study was aimed at assessing the effectiveness of an integrated intensive lifestyle intervention (ILI) in Indian patients with prediabetes while exploring sex- and body mass index (BMI)–based differences.Methods: This retrospective study analyzed data from 427 patients with prediabetes (HbA1c: 5.7%–6.4% not on insulin or oral hypoglycemic agents and aged 18–75 years) who underwent a 1-year online ILI program at the Freedom from Diabetes Clinic, India, between 2020 and 2023. The intervention consisted of a personalized plant-based diet, physical activity, psychological support, and medical management. Anthropometric and biochemical data were extracted from the clinical database, and logistic regression was used to identify factors associated with prediabetes remission.
Results: At the end of the study, 47.1% of patients achieved prediabetes remission. Significant weight loss and improvements were observed in HbA1c, BMI, fasting blood glucose, fasting insulin, insulin resistance, lipid profile, and blood pressure (p < 0.05). Notably, 34% of patients lost > 10% of their body weight. Females achieved greater reductions in weight and BMI than males (p < 0.001). The BMI stratified analysis revealed higher remission rates in the obesity group (BMI ≥ 25 kg/m2) (49.9%) than in the nonobesity group (BMI 18–24.9 kg/m2) (37.0%) (p = 0.028). The obesity group showed greater improvements in glycemic parameters and insulin resistance than the non-obesity group (p < 0.05). Logistic regression identified age ≤ 50 years (OR: 2.15, 95% CI: 1.42–3.27), endline HOMA-IR < 2.5 (OR: 1.60, 95% CI: 1.01–2.45), and > 10% weight loss (OR: 3.72, 95% CI: 2.34–5.90) as significant factors associated with prediabetes remission.
Conclusions: Prediabetes remission was achieved in almost half of the patients, highlighting the effectiveness of a tailored multidisciplinary approach for managing prediabetes in the Indian population. The study showed significant weight loss, improved glycemic control, and better lipid profiles and emphasized the need for personalized strategies for prediabetes management considering factors such as sex and BMI.
Trial Registration: Clinical Trials Registry of India identifier: CTRI/2024/03/064596
-
Retrospective Evaluation of the Impact of a Multidisciplinary One-Year Online Lifestyle Intervention on Type 2 Diabetes Remission in Nonobese Indian Patients
Abstract:
Background and Objective: Despite the high prevalence of T2D among nonobese Indians, there is a notable lack of comprehensive lifestyle intervention studies that target this population. This retrospective study was aimed at filling this gap by evaluating the impact of a multidisciplinary 1-year online intensive lifestyle intervention (ILI) on T2D remission in nonobese Indian patients.
Methodology: Retrospective data from medical records of 1453 nonobese patients (BMI 18.5–24.9 kg/m2) (aged > 18 years) who participated in a 1-year online subscription-based ILI program at the Freedom from Diabetes Clinic, India, between June 2020 and October 2023 were extracted for analysis. The program included a plant-based diet, physical activity regimens, psychological support, and medical management. Homeostatic model assessment of insulin resistance (HOMA2-IR) and beta cell function (HOMA2%B) were calculated. Remission was defined as maintaining glycated hemoglobin (HbA1C) < 6.5%, measured at least 3 months after cessation of glucose-lowering pharmacotherapy.
Results: The study included 1453 patients (72% male), with a median age of 53 years (IQR: 15), BMI of 23 kg/m2 (IQR: 2.2), and diabetes duration of 10.5 years (IQR: 10.4). Postintervention, significant changes were observed, including a reduction in weight (−1.5 kg), fasting blood glucose (−13.2 mg/dL), fasting insulin (−0.4 μU/mL), HOMA2-IR (−0.07), and HbA1c (−1.2%), along with an increase in HOMA2%B (+3.1) (p < 0.05). Remission was observed in 24% of the patients. The study identified the baseline predictors of remission as being over 40 years of age at onset, having a diabetes duration of less than 6 years, maintaining good glycemic control (HbA1C ≤ 7%), and being drug-naïve. Postintervention factors, such as weight loss and improved beta-cell function, were also significant predictors of remission (p < 0.05).
Conclusion: These findings suggest that a multidisciplinary lifestyle intervention program can significantly improve glycemic control and promote T2D remission in nonobese Indian patients in a real-world setting, thereby highlighting the importance of early intervention and weight management in this population.
Trial Registration: Clinical Trials Registry of India identifier: CTRI/2024/03/064596
-
Baseline clinical and biochemical profiles of type 2 diabetes patients enrolled in a lifestyle management program in India, a cross-sectional study
Abstract:
Assessing the clinical and biochemical profiles of patients with type-2 diabetes (T2D) is vital for understanding the disease characteristics and improving disease management. This study aimed to assess the profiles of adults (> 18 years old) with T2D enrolled in a one-year diabetes management program in Pune, India. This cross-sectional study retrospectively analyzed 18,950 records from the Freedom from Diabetes Clinic, between November 2015 and June 2023. Baseline sociodemographic, biochemical, and anthropometric parameters were extracted from electronic medical records and analyzed using descriptive statistical methods. A gender-wise comparison was performed for the biochemical and anthropometric measurements. Poor glycemic control (glycated hemoglobin [HbA1c] ≥ 7%) was reported by 70.0% of the patients at baseline, despite the majority (80.2%) being on glucose lowering medications. The prevalence of overweight (body mass index [BMI] 23.0–24.9 kg/m2) and obesity (BMI ≥ 25 kg/m2) was 21.5% and 57.2%, respectively. Hypertension and hypercholesterolemia were reported in 56.8% and 25.7% of the patients, respectively. A significant association was observed between comorbidities such as hypertension, overweight/obesity, and poor glycemic control (p < 0.05). Additionally, significant gender-wise differences were observed in the clinical parameters, including homeostatic model assessment of insulin resistance, fasting insulin, and micronutrients (p < 0.05). This study highlights the high prevalence of poor glycemic control, overweight/obesity, and comorbidities among T2D patients enrolled in a one-year diabetes management program in India. Gender-specific differences emphasize the need for tailored management approaches. These findings underscore the importance of comprehensive lifestyle interventions to improve glycemic control, address comorbidities, and reduce complication risks in the Indian population with T2D. -
Type 2 diabetes remission through lifestyle intervention in a geriatric patient with long-standing diabetes and at thirty-three-months follow-up
Summary: Type 2 diabetes (T2D) is a chronic metabolic disorder that affects millions of people worldwide, particularly the elderly population. Remission of T2D in elderly patients through lifestyle modifications has been well documented, especially in newly diagnosed patients with good glycemic control and without obesity. It is also common in patients with obesity undergoing bariatric surgery. In this report, we present the case of a 66-year-old male patient with a 30-year history of T2D and mild obesity who achieved remission of T2D through customized integrated intensive lifestyle modifications, including a vegan diet, exercise and psychological support. The patient showed an improvement in HbA1c (7.7 to 5.3%) and insulin resistance (HOMA-IR; 6.2 to 1.8) and a shift in BMI (25.3 to 23.7 kg/m2) through weight loss (73 to 67 kg). The patient remains in remission 33 months after the completion of the intervention. This case suggests the possibility of long-term remission with lifestyle changes in patients with advanced age, a longer duration of diabetes and mild obesity.
Learning points: Long-term sustained remission is possible in a geriatric patient with long-standing type 2 diabetes (T2D) of more than 30 years. Customized integrated intensive lifestyle intervention can lead to a significant improvement in glycemic control and insulin resistance in elderly patients with T2D. Integrated lifestyle interventions, including a vegan diet, exercise and psychological support, have the potential to stop the usage of oral hypoglycemic agents and insulin in an elderly patient with a prolonged history of T2D and mild obesity.
Keywords: diabetes remission; geriatric patients; lifestyle intervention; long-standing type 2 diabetes; mild obesity.
-
Psychometric validation of type 2 Diabetes Distress Assessment System in an Indian type 2 diabetes population
Abstract
Diabetes distress (DD) significantly burdens and negatively impacts self-management and health outcomes in patients with type 2 diabetes (T2D). Early detection and management of DD are crucial for effective T2D management. The Diabetes Distress Assessment System (T2-DDAS) is a recently validated tool for measuring DD, but its psychometric properties in non-Western populations, such as India, have not been evaluated. This study aimed to assess the validity and reliability of T2-DDAS in Indian patients with T2D. Data from 408 T2D patients enrolled in a one-year diabetes management program at the Freedom from Diabetes Clinic in Pune, India, from January to March 2024, were analyzed. Sociodemographic characteristics, medical history, and anthropometric parameters were extracted from existing records. T2-DDAS, previously validated in a Western population, was administered. Statistical analyses included descriptive statistics, Principal Component Analysis (PCA), Exploratory Factor Analysis (EFA), Confirmatory Factor Analysis (CFA), and Structural Equation Modeling (SEM), using IBM SPSS, R, and AMOS software. The T2-DDAS demonstrated good internal consistency (Cronbach’s α = 0.91). CFA yielded satisfactory fit indices (χ² = 1036.92, RMSEA = 0.07, TLI = 0.905, CFI = 0.918), supporting the construct validity of T2-DDAS for the Indian population. The T2-DDAS is a valid and reliable tool for assessing DD in Indian patients with T2D. -
Improvement in symptoms of anxiety and depression in individuals with type 2 diabetes: retrospective analysis of an intensive lifestyle modification program
Abstract
Background
Type 2 diabetes (T2D) is a chronic metabolic disorder that has a notable influence on mental well-being, contributing to elevated morbidity and mortality rates. Depression and anxiety disorders are the most common mental health concerns among patients with T2D worldwide. Therefore, the present study aimed to assess the impact of an online intensive lifestyle intervention (ILI) on mental health outcomes (depression and anxiety) in patients with T2D in India.
Materials and methods
This retrospective pre-post analysis included adult patients (aged > 18 years) diagnosed with T2D who were enrolled in a diabetes management program in India between June 2021 and June 2023. The intervention consisted of lifestyle modifications such as a customized plant-based diet, regular physical activity, psychological support through group and individual therapy, and medical management. Data were extracted from the electronic database of the clinic, including anthropometry, medical history, biochemical parameters, symptoms of depression, and anxiety (assessed using the Patient Health Questionnaire-9 (PHQ-9) and Generalized Anxiety Disorders-7 (GAD-7) scale) at the start and end of the six-month intervention period.
Results
Of the 1061 eligible patients (177 with prediabetes), 40.3% were female. The mean age, duration of diabetes, and HbA1c levels were 52 ± 10.4 years, 9.8 ± 7.8 years, and 8 ± 1.7%, respectively. The prevalence of symptoms of depression and anxiety (ranging from mild to severe) was 46% and 44.3%, respectively, which reduced to 28.7% and 29.2%, respectively, post-intervention.
Conclusion
Integrated ILI successfully improved the symptoms of anxiety and depression, highlighting the importance of a multidisciplinary approach that includes diet, physical activity, psychological support, and medical management in enhancing mental health outcomes among patients with T2D. Future prospective studies are needed to explore the long-term effects of such interventions and develop effective strategies for promoting mental health in diverse populations. -
Diabetes Remission After Radical Nephrectomy in a Geriatric Patient With Obesity and Type 2 Diabetes—34 Months’ Follow-Up
Abstract
Diabetes mellitus significantly affects survival in patients with renal cell carcinoma undergoing nephrectomy, requiring personalized care. This case involved a 64-year-old man with type 2 diabetes (T2D) who underwent radical nephrectomy for renal cell carcinoma. He consented to a 1-year intensive lifestyle intervention (ILI), including a vegan diet (to lower calorie intake, reduce uric acid, support renal health, and promote weight loss), intermittent fasting, regular exercise, psychological support, and medical management. Quarterly biochemical assessments and monthly adherence evaluations were conducted. Post intervention, the patient achieved diabetes remission, maintaining glycated hemoglobin A1c (HbA1c) below 6.5% (48 mmol/mol) (reference range, <6.5%; <48 mmol/mol) without medication. He lost 36 kg (79.37 lb), reducing his body mass index from 35.3 to 25.1. His lipid profile normalized (total cholesterol, 175 to 127 mg/dL (4.53 to 3.29 mmol/L) (reference range, <200 mg/dL; <5.18 mmol/L); triglycerides, 155 to 73 mg/dL (1.75 to 0.82 mmol/L) (reference range, <150 mg/dL; <1.69 mmol/L), allowing the discontinuation of statins. Improvements in serum creatinine and high-sensitivity C-reactive protein levels were also observed. The patient exhibited normal glucose tolerance, consecutively passing an oral glucose tolerance test for 2 years. This case highlights the potential of lifestyle modifications in managing T2D in patients with a history of nephrectomy. -
Comparison of clustering and phenotyping approaches for subclassification of type 2 diabetes and its association with remission in Indian population
Abstract
Identification of novel subgroups of type 2 diabetes (T2D) has helped improve its management. Most classification techniques focus on clustering or subphenotyping but not on both. This study aimed to compare both these methods and examine the rate of T2D remission in these subgroups in the Indian population. K-means clustering (using age at onset, HbA1C, BMI, HOMA2 IR and HOMA2%B) and subphenotyping (using homeostatic model assessment (HOMA) estimates) analysis was done on the baseline data of 281 patients with recently diagnosed T2D who participated in a 1-year online diabetes management program. Cluster analysis revealed three distinct clusters: severe insulin-deficient diabetes (SIDD), severe insulin-resistant diabetes (SIRD), and mild obesity-related diabetes (MOD) while subphenotyping showed four distinct categories: hyperinsulinemic, insulinopenic, classical, and nascent T2D. Comparison of the two approaches revealed that the clusters aligned with phenotypes based on shared characteristics of insulin sensitivity (IS) and beta cell function (BCF). Clustering correctly identified individuals in nascent group (high IS and BCF) as having mild obesity related diabetes which subphenotyping did not. Post-one-year intervention, higher remission rates were observed in the MOD cluster (p = 0.383) and the nascent phenotype showing high IS and BCF (p = 0.061, Chi-Square test). In conclusion, clustering based on a comprehensive set of parameters appears to be a superior method for classifying T2D compared with pathophysiological subphenotyping. Personalized interventions may be highly effective for newly diagnosed individuals with high IS and BCF and may result in higher remission rates in these individuals. Further large-scale studies are required to validate these findings. -
The Diabetes Remission in India (DiRemI) study: Protocol for a prospective matched-control trial
Background
The global rise in diabetes, particularly in India, poses a significant public health challenge, with factors such as limited awareness, financial strain, and cultural considerations hindering its effective management. Although lifestyle changes have shown promising results, their consistent implementation and maintenance continue to pose challenges. Most studies have focused primarily on dietary modifications, overlooking other essential aspects of lifestyle intervention. The DiRemI study aims to address these gaps by evaluating the efficacy of a comprehensive one-year program that combines diet, exercise, psychological support, and medical management to achieve weight loss, diabetes remission, and improved glycemic control among patients with type 2 diabetes (T2D) in India, while also considering the unique needs of the Indian population.Methods
The DiRemI study is a prospective, open-label, matched-group trial aimed at assessing the impact of a one-year online integrated intensive lifestyle intervention (ILI) comprising dietary modifications, physical activity, psychological support, and medical management on weight loss and remission in adult T2D patients (aged 30–70 years), with a body mass index (BMI) between 25 and 35 kg/m2, and disease duration of <15 years. ILI will be compared with routine medical care (RMC). Participants will be recruited from three clinics: one providing ILI and two others providing RMC. The co-primary outcome will be weight loss and remission at 12 months, with a follow-up at 18 months. The proposed sample size is 360 participants (180 each in intervention and control group).Discussion
The DiRemI study represents the first large-scale remission study in India to show the effectiveness of an integrated approach in the remission and management of T2D and its complications. The findings of this study hold the potential to report evidence-based strategies for managing T2D both in India and globally, thus alleviating the substantial burden of diabetes on public health systems. -
Interplay Between the American Diabetes Association’s ABC Targets for Diabetes, Insulin Resistance Indices, and Dyslipidemia in Indian Type 2 Diabetes Patients
Background
The increasing incidence of type 2 diabetes (T2D) in India underscores the pressing need for effective management strategies. Meeting the American Diabetes Association (ADA) ABC targets for diabetes (glycated hemoglobin (HbA1c), blood pressure, and serum low-density lipoprotein cholesterol (LDL-C)) is crucial for effectively managing T2D, as it reflects the optimal control of key metabolic parameters. Insulin resistance (IR) and impaired beta cell function (BCF) have been found to have a significant impact on glycemic control, lipid metabolism, and hypertension, contributing to the complex cardiovascular risk profile of patients with T2D. This study aimed to explore the association between ABC targets for diabetes, IR, BCF, and dyslipidemia in a cross-sectional cohort of T2D patients.Methods
This retrospective study examined data from 681 T2D patients with comorbid hypertension and dyslipidemia. The patients were part of a one-year online lifestyle intervention program for diabetes management at the Freedom from Diabetes Clinic in Pune, India, between January 2021 and December 2022. Baseline data (at the time of enrollment in the program) on medical history and anthropometric and biochemical parameters were retrospectively extracted from medical records and used to assess ABC targets and other clinical parameters. The ABC targets for diabetes include three goals: an HbA1c level of less than 7.0%, a blood pressure level of less than 140/90 mmHg, and an LDL-C level of less than 100 mg/dL. Homeostatic Model Assessment of Insulin Resistance (HOMA-IR), Homeostatic Model Assessment of Beta Cell Function (HOMA-B), and Quantitative Insulin Sensitivity Check Index (QUICKI) were calculated using standard formulas.Results
Cross-sectional analysis at baseline showed that 152 (22.3%) participants met all three ABC targets, 306 (45.0%) and 183 (26.8%) participants met two or one targets, respectively, and 40 (5.9%) did not meet any of the ABC targets. Participants meeting all three targets showed significantly lower IR, higher sensitivity (HOMA-IR, median 2.1; QUICKI, median 0.34), higher BCF (HOMA-B, median 62.9), and healthier lipid profiles (mg/dL) (total cholesterol, median 126; triglycerides, median 114; and non-high-density lipoprotein (HDL), median 84) than those who did not meet any of the ABC targets (HOMA-IR, median 3.4; QUICKI, median 0.31; HOMA-B, median 31.7; total cholesterol, median 221; triglycerides, median 187; and non-HDL, median 182) (p < 0.01). A significant association was observed between lower BMI (< 25 kg/m2), lower IR (HOMA-IR <2.5), and meeting all three ABC targets (p < 0.01). No significant association was observed between the duration of diabetes and ABC target status (p > 0.1). Lower IR was identified as a predictor of achievement of all three ABC targets (p < 0.01).Conclusion
This study highlights the significance of meeting ABC targets for diabetes in relation to not only a better lipid profile but also lower IR and higher BCF. These preliminary findings provide novel insights into the interplay between IR, BCF, dyslipidemia, and meeting ABC targets in an Indian T2D population. These findings highlight the need for effective diabetes management strategies and improved patient outcomes, considering factors such as BMI and IR indices. -
Oral glucose tolerance test clearance in type 2 diabetes patients who underwent remission following intense lifestyle modification: A quasi-experimental study
Achieving diabetes remission (HbA1c<48mmol/mol without the use of anti-diabetic medication for 3 months) might not assure restoration of a normal glycemic profile [fasting blood sugar level <5.6 mmol/L and Post-Prandial (PP) blood glucose <7.8mmol/L]. The study investigates the factors associated with OGTT clearance in patients under type 2 diabetes remission. Four hundred participants who achieved remission during a one-year online structured lifestyle modification program, which included a plant-based diet, physical activity, psychological support, and medical management (between January 2021 and June 2022), and appeared for the OGTT were included in the study. OGTT clearance was defined by fasting blood glucose < 5.6 mmol/L and 2-hour post-prandial blood glucose <7.8 mmol/L post-consumption of 75g glucose solution. Of the 400 participants, 207 (52%) cleared OGTT and 175 (44%) had impaired glucose tolerance (IGT). A shorter diabetes duration (<5 years) was significantly associated with OGTT clearance (p<0.05). Pre-intervention use of glucose-lowering drugs showed no association with OGTT clearance (p>0.1). Post-intervention, the OGTT-cleared group showed significantly higher weight loss (p<0.05) and a decrease in HbA1c compared to the IGT group (p<0.05). Improvement in Insulin resistance and β-cell function was also higher in the OGTT-cleared group compared to the IGT group (p<0.05). In conclusion, clearing the OGTT is a possibility for those achieving remission through lifestyle interventions. Higher weight loss, a shorter duration of diabetes, and improvement in insulin resistance were significantly associated with OGTT clearance in participants in remission. Future randomized controlled trials with longer follow-ups may help substantiate our findings.
-
Prevalence and Predictors of Anxiety and Depression in Indian Patients with Type 2 Diabetes
Background
Numerous investigations indicate the presence of a reciprocal association between type 2 diabetes (T2D) and a range of mental health conditions. However, research on the factors that contribute to depression and anxiety in T2D patients in India is scarce.Purpose
The present study aims to identify the prevalence and predictors of depression and anxiety in patients with T2D in India.Methods
A cross-sectional study that included 2,730 patients with T2D was conducted at the Freedom from Diabetes Clinic in Pune, India. Anxiety and depression were measured by the Patient Health Questionnaire-9 (PHQ-9) and Generalized Anxiety Disorders-7 (GAD-7) Scale. Binary logistic regression was applied to identify the factors predicting anxiety and depression.Results
The prevalence of depression and anxiety were 20.3% and 17.3%, respectively. The major predictors of anxiety and depression were female gender, obesity, unmarried marital status, poor glycaemic control and the presence of comorbid conditions.Conclusion
This study’s findings highlight a significant prevalence of depression and anxiety among patients with T2D in India, with key predictors including gender, obesity, marital status, glycaemic control and comorbid conditions. These findings highlight the critical need for integrated mental health support in routine diabetes care to manage depression and anxiety. -
A Rare Case of Type 2 Diabetes Remission Following Non-Pharmacological Intense Lifestyle Modification in a Liver Transplantation Recipient: A Case Report
Solid organ transplantation, especially liver transplantation, is higher in patients with Type 2 Diabetes (T2D), with further worsening of glycemic control post-transplantation. This vicious cycle increases the risk of cardiovascular mortality, emphasizing the need for an effective T2D management strategy. We present a unique case of T2D remission through intensive lifestyle modification in a liver transplant recipient. A 55-year-old male liver transplant recipient with a history of T2D since 1995 and insulin therapy for 17 years experienced severe non-alcoholic fatty liver disease (NAFLD) and liver cirrhosis, necessitating a liver transplant in 2016. Post-transplant, he was on insulin and immuno-suppressants. In 2021, the patient joined our one-year diabetes management program, involving intense lifestyle modifications, including a plant-based, low- carbohydrate diet, physical activity, stress management, mindfulness meditation, and medical management. Insulin dose adjustments were made based on daily glucose monitoring. After three months, the patient experienced hypoglycemia, and insulin was discontinued. T2D remission was confirmed by normal blood glucose levels and an HbA1c of 6.3% and clearing of oral glucose tolerance tests (OGTT) twice post remission (at 9 and 21 months). This case report provides the first-ever documented evidence of T2D remission through non-pharmacological intervention after liver transplantation. Additionally, it reports the first-ever OGTT clearance following T2D remission post-liver transplantation.
Keywords: Diabetes remission, lifestyle intervention, liver transplantation, type 2 diabetes. -
Lifestyle Intervention for Diabetes Remission: A Paradigm Shift in Diabetes Care and Management
Journal: Current Diabetes Reviews, Online Ahead of PrintRemission is often considered the ultimate goal in Type 2 Diabetes (T2D) management and care. Although metabolic surgery is the conventional choice to achieve remission, substantial evidence suggests the possibility of T2D remission through lifestyle interventions. In this context, the current perspective explores recent scientific advancements in lifestyle intervention for diabetes remission and also emphasises its clinical applicability as a pragmatic approach to diabetes management. The perspective further provides additional evidence on remission from the authors' own research findings in the Indian population. We propose that a holistic lifestyle intervention approach - individualised diet plan, exercise protocol, and psychological intervention - may be a benchmark protocol to achieve T2D remission.
-
Long‑term remission of type 2 diabetes through intense lifestyle modification program–A case series
Journal of Family Medicine and Primary Care, September 2023, Vol. 12Type 2 diabetes (T2D) remission is being widely accepted and documented as feasible through calorie restriction and bariatric surgery.
Recent studies with lifestyle changes have also shown T2D remission; however, long‑term remission through lifestyle modifications is not yet established. Though glycated hemoglobin (HbA1c) is a universally accepted indicator of glycemic status, oral glucose tolerance test (OGTT) would be a more robust marker in understanding whether the metabolic abnormalities in glucose metabolism have undergone complete remission as well. We present a case series of four patients enrolled in the Holistic Transformation Program, a lifestyle modification program, between 2016 and 2018. The intervention was a combination of a vegan diet, structured exercises, and stress management delivered over 12 months. All four patients successfully achieved T2D remission and cleared OGTT consecutively for a minimum period of 3 years. Our findings suggest that long‑term T2D remission may be possible through lifestyle modification. -
Type 2 Diabetes Remission Through Intense Lifestyle Modification with Three-Year Follow-Up of an Elderly Male on High Insulin Dosage: A Case Report
Integrative Medicine (Encinitas), September 2023, Vol. 22, No. 4An elderly obese male patient (60 yrs.) diagnosed Type 2 Diabetes (T2D) presented to our clinic. He was on 94 units of insulin and oral hypoglycemic agents during his initial consultation visit. After obtaining informed consent, he was enrolled into intense lifestyle modification program for a duration of six months, with a three-year follow-up after the intervention. The patient underwent complete remission losing 13 kg of body weight and also successfully clearing oral glucose tolerance tests (OGTT) for three consecutive years. We present three unique features in the current case report:
(1) Elderly age of the patient
(2) OGTT clearance along with normalisation of HbA1c, and
(3) High initial insulin dosage at baseline.
A few of the common positive predictors of T2D remission documented in earlier studies include younger age and minimal or low doses of insulin. The current case study shows that older age and higher dosage of insulin, it is possible to undergo complete T2D remission along with OGTT clearance through intense holistic lifestyle modification.
Future experimental studies with adequate sample sizes would help substantiate our observation. -
Extent of Diabetic Nephropathy Reversal in Type 2 Diabetes Mellitus Patients by following the Freedom from Diabetes Protocol
Indian Journal of Public Health Research & Development, August 2020, Vol. 11, No. 8Introduction The purpose of the study is to test the efficacy of Freedom from Diabetes (FFD) protocol on diabetic nephropathy patients.
Methods Out of 776 participants enrolled, 302 had diabetic nephropathy. Selected participants were given a specially modified plant based diet along with lymphatic movement, anti-gravity exercises and relevant supplements to reverse the effects of nephropathy. Baseline characteristics, anthropometric measurements and biochemical parameters were measured on visit 1 and visit 2.
Results - After 6 months, there was a significant reduction in urinary microalbumin and serum creatinine levels which was accompanied by improvement in glycemic control. Anthropometric measurements like body weight and BMI also showed a significant improvement.
Conclusion - This study states that FFD protocol (specifically adapted plant-based diet along with lymphatic movement and anti-gravity exercises) with relevant supplements helps in improving diabetic nephropathy status.
-
Reversal of Metabolic Syndrome With Plant Based Diet And Exercise: Case Report
Journal: Ayushdhara, March - April 2020, Vol 7, Issue 2This study aimed to investigate the effectiveness of a specified diet pattern and exercise like lymphatic and strength-building exercises (FFD protocol) to enhance weight and fat loss. A 45-year-old male with a history of obesity and diabetes mellitus (DM) enrolled in the study. The patient followed a specified diet along with lymphatic and strength-building exercises. Follow up was done for 6 months where, baseline characteristics, anthropometric measurements and biochemical parameters were measured in visit 1 and visit 2. The patient was off DM medication in 10 days. In first follow up (3 months) weight, BMI, waist circumference and body fat was significantly reduced. Whereas skeletal muscle mass was increased. A drop in HbA1C, fasting insulin, fasting blood sugar level and postprandial blood sugar levels were observed. In comparison to first follow up the second follow up after 6 months, shows substantial changes in the basal parameters. A drastic decline in HbA1c was reported from 6.1% to 5.5%. The FFD program comprehensively targets diabetes, ultimately clearing GTT the harbinger of the defeat of diabetes and visceral obesity, thereby successfully reversing the cluster of components of this morbid syndrome.
Scientific Conferences
INTERNATIONAL
-
World Congress of Diabetes 2026 (Diabetes India) | Hyderabad | 13th -15th February 2026

1] Effectiveness of Comprehensive Lifestyle Interventions in Meeting American Diabetes Association’s ABC (HbA1c, Blood pressure, and LDL-C) Targets Among Indian Patients with Type 2 Diabetes
Authors: Diptika Tiwari, Pramod Tripathi, Nidhi Kadam, Baby Sharma, Thejas Kathrikolly, Anagha Vyawahare, Malhar Ganla, Banshi Saboo
2] Sustained Insulin Independence in an Elderly Patient with Long-Standing Type 2 Diabetes Following an Intensive Lifestyle Intervention: A 5-Year Follow-up Case Report
Authors: Thejas Kathrikolly, Pramod Tripathi, Nidhi Kadam, Anagha Vyawahare, Baby Sharma, Diptika Tiwari, Malhar Ganla, Banshi Saboo
3] Visceral Fat Reduction as a Key Predictor of Type 2 Diabetes Remission in Patients with Obesity: A One-Year Lifestyle Intervention Study
Authors: Anagha Vyawahare, Pramod Tripathi, Nidhi Kadam, Diptika Tiwari, Baby Sharma, Thejas Kathrikolly, Malhar Ganla, Banshi Saboo
4] Multidisciplinary Lifestyle Intervention Improves Metabolic and Mental Health Outcomes in Indian Adults with Diabesity
Authors: Baby Sharma, Pramod Tripathi, Nidhi Kadam, Diptika Tiwari, Thejas Kathrikolly, Anagha Vyawahare, Malhar Ganla, Banshi Saboo -
ACLM Annual Conference 2025 (American College of Lifestyle Medicine) | Grapevine, Texas | 16th-19th November 2025

1] Sustained Type 2 Diabetes Remission through Intensive Lifestyle Intervention: An Eight-Year Follow-Up Case Report
Authors: Nishikant Bhanagay, Nidhi Kadam, Pramod Tripathi, Baby Sharma
2] Role of Progressive Intermittent Fasting in Type 2 Diabetes Women with Overweight and Obesity
Authors: Pramod Tripathi, Diptika Tiwari, Nidhi Kadam, Anagha Vyawahare Baby Sharma, Thejas Kathrikolly, Nishikant Bhanagay
3] Effectiveness of Lifestyle Intervention in Type 2 Diabetes with Chronic Kidney Disease
Authors: Nidhi Kadam, Anagha Vyawahare, Pramod Tripathi, Diptika Tiwari, Baby Sharma, Thejas Kathrikolly, Manisha Shah
4] Reduced Dependence on Antihyperglycemic Therapy in a Geriatric Patient with Longstanding Diabetes through an Intensive Lifestyle Intervention – A Case Report with 56 months Follow-up
Authors: Manisha Shah, Pramod Tripathi, Nidhi Kadam, Thejas Kathrikolly -
American Heart Association (AHA) | Chicago, USA | 8th – 10th November 2025

Abstract No.4365737: Title: Intensive Lifestyle Intervention Strategies for Improving Atherogenic Profile and Estimated Cardiovascular Risk in Indian Adults with Obesity
Authors: Pramod Tripathi, Diptika Tiwari, Nidhi Kadam, Akiva Rosenzveig, Anmol Multani, Faysal Massad, Aravinda Nanjundappa
View journal -
EASD 2025 | European Association for the Study of Diabetes | Vienna, Austria | 15th – 19th September 2025

Impact of a Multidisciplinary Lifestyle-based Diabetes Management Program on Physical and Mental Health Outcomes in Indian Type 2 Diabetes Individuals Living with Obesity
Authors: Baby Sharma, Pramod Tripathi, Malhar Ganla, Anagha Vyawahare, Thejas Kathrikolly, Diptika Tiwari, Banshi Saboo, Nidhi Kadam
Optimizing American Diabetes Association’s ABC target (HbA1c, blood pressure, and LDL-C) achievement in Type 2 Diabetes through lifestyle interventions: An Indian study
Authors: Diptika Tiwari, Pramod Tripathi, Nidhi Kadam, Anagha Vyawahare, Baby Sharma, Thejas Kathrikolly, Malhar Ganla, Banshi Saboo
Impact of an Integrated Lifestyle Intervention on Body Composition and Type 2 Diabetes Remission: The Key Role of Visceral Fat Reduction
Authors: Pramod Tripathi, Anagha Vyawahare , Nidhi Kadam, Diptika Tiwari, Baby Sharma, Thejas Kathrikolly, Malhar Ganla, Banshi Saboo -
ADA 2025 | American Diabetes Association | Chicago, IL | 20th - 23rd June 2025

Impact of Online Supervised Nine-Day Progressive Fasting Program on Anthropometric and Glycemic Outcome in Patients with Type 2 Diabetes Free
Authors:Pramod Tripathi; Baby Sharma; Nidhi S. Kadam; Diptika Tiwari; Anagha R. Vyawahare; Thejas Kathrikolly; Malhar H. Ganla; Banshi D. Saboo
View journal
Enhancing ABC Target Achievement in Type 2 Diabetes through Integrated Intensive Lifestyle Interventions—A One-Year Study in an Indian Population Free
Authors: Pramod Tripathi; Diptika Tiwari; Nidhi S. Kadam; Thejas Kathrikolly; Baby Sharma; Anagha R. Vyawahare; Malhar H. Ganla; Banshi D. Saboo
View journal -
ECO-EASO 2025 | European Congress on Obesity | Malaga, Spain | 11th – 14th May 2025

Intensive Lifestyle Intervention Strategies for Improving Cardiovascular Risk in Indian Adults with Obesity
Authors: Diptika Tiwari, Pramod Tripathi, Nidhi Kadam, Baby Sharma, Anagha Vyawahare, Thejas Kathrikolly, Malhar Ganla, Banshi Saboo
Impact of a Multidisciplinary Lifestyle-based Obesity Management Program on Physical and Mental Health Outcomes in Indian Adults Living with Obesity
Authors: Baby Sharma, Pramod Tripathi, Malhar Ganla, Diptika Tiwari, Thejas Kathrikolly, Anagha Vyawahare, Banshi Saboo, Nidhi Kadam
Improving Body Composition and Diabetes Outcomes through Structured Lifestyle Interventions in Indian Women with Type 2 Diabetes
Authors: Anagha Vyawahare, Pramod Tripathi, Nidhi Kadam, Diptika Tiwari, Baby Sharma, Thejas Kathrikolly, Malhar Ganla, Banshi Saboo -
IDF 2025 | International Diabetes Federation | Bangkok, Thailand | 07th – 10th April 2025
Subclassification of Type 2 Diabetes in Drug-Naive Patients and Its Impact on Remission Post-Lifestyle Intervention
Authors: Pramod Tripathi, Anagha Vyawahare, Nidhi Kadam, Diptika Tiwari, Baby Sharma, Thejas Kathrikolly, Malhar Ganla, Banshi Saboo -
Diabetes India 2025 | World Congress of Diabetes | Ahmedabad, India | 13th – 16th February 2025

Psychometric Burden in Indian Type 2 Diabetes Patients: Prevalence and Predictors of Distress, Depression, and Anxiety
Authors: Baby Sharma, Pramod Tripathi, Nidhi Kadam, Diptika Tiwari, Thejas Kathrikolly, Anagha Vyawahare, Malhar Ganla, Banshi Saboo
Enhancing Metabolic Health in Women with Type 2 Diabetes: The Role of Intermittent Fasting and Lifestyle Intervention
Authors: Diptika Tiwari, Pramod Tripathi Nidhi Kadam, Baby Sharma, Thejas Kathrikolly, Anagha Vyawahare, Malhar Ganla, Banshi Saboo -
American Heart Association (AHA) | Chicago, USA | 16th – 18th November 2024

Abstract 4144878: Comparison of Glycemic Profile, Cardiovascular Risk Factors, and Insulin Resistance in Type 2 Diabetic Patients with Metabolic Syndrome: A Retrospective Analysis
Authors: Pramod Tripathi, Lidiya Sul, Matthew Lee, Aravinda Nanjundappa, Samir Kapadia, Dipitka Tiwari, Nidhi Kadam
View journal
Abstract 4142028: An Intensive Lifestyle Intervention Improves Cardiovascular Health Outcomes in Patients with Type-2 Diabetes
Authors: Pramod Tripathi, Thejas Kathrikolly, Lidiya Sul, Matthew Lee, Aravinda Nanjundappa, Samir Kapadia, Nidhi Kadam
View journal -
ACLM Annual Conference 2024 (American College of Lifestyle Medicine) | Orlando, FL | 27th-30th October 2024

Diabetes Remission with Intensive Lifestyle Intervention after Radical Nephrectomy in a Geriatric Patient with Obesity and Type 2 Diabetes - Case Report with a 34-Month Follow-up
Authors: Authors: Manisha Shah, Pramod Tripathi, Nidhi Kadam, Baby Sharma, Diptika Tiwari, Malhar Ganla
Body fat loss and skeletal muscle mass gain are associated with diabetes remission post-integrated lifestyle intervention in Indian population
Authors: Nidhi Kadam, Pramod Tripathi, Anagha Vyawahare, Diptika Tiwari, Baby Sharma, Thejas Kathrikolly, Manisha Shah
Type 2 Diabetes Remission in an Elderly Patient with Obesity and Long-Standing Diabetes through Customized Lifestyle Intervention
Authors: Nishikant Bhanagay, Pramod Tripathi, Nidhi Kadam, Diptika Tiwari, Baby Sharma
Integrated Lifestyle Intervention for Weight Loss and Improvement in Cardiovascular Risk and Glycemic Parameters among Patients with Type 2 Diabetes
Authors: Pramod Tripathi, Thejas Kathrikolly, Nidhi Kadam, Diptika Tiwari, Baby Sharma, Anagha Vyawahare, Manisha Shah -
60th European Association for the Study of Diabetes (EASD) | Madrid, Spain | 9th – 13th September 2024

Abstract no 363: Prediabetes Management in Indian Adults: A Quasi-Experimental Study On Effectiveness Of Integrated Intensive Lifestyle Intervention
Authors: Malhar Ganla, Pramod Tripathi, Diptika Tiwari, Nidhi Kadam, Anagha Vyawahare, Baby Sharma, Thejas Kathrikolly, Bansi Saboo
View journal -
ADA 2024 | American Diabetes Association | Orlando, Florida | 21st -24th June 2024

Beta Cell Function Is a Stronger Predictor Than Insulin Resistance for Development of Type 2 Diabetes in Obese Indian Population: A Matched-Pair Cohort Analysis
Authors: Pramod Tripathi; Nidhi S. Kadam; Anagha R. Vyawahare; Thejas Kathrikolly; Diptika Tiwari; Baby Sharma; Malhar H. Ganla; Mamata Hiremath; Banshi D. Saboo
View journal
Prevalence and Determinants of Diabetes Distress in Type 2 Diabetes Patients in India: A Cross-Sectional Study
Authors: Pramod Tripathi, Nidhi Kadam, Baby Sharma, Pournima Kulkarni, Mayurika Das Biswas, Malhar Ganla, Banshi Saboo
View journal
Effectiveness of Freedom from Diabetes Protocol in managing prediabetes in Indian population: A quasi-experimental study
Authors: Pramod Tripathi; Nidhi S. Kadam; Diptika Tiwari; Anagha R. Vyawahare; Baby Sharma; Thejas Kathrikolly; Malhar H. Ganla; Mamata Hiremath; Banshi D. Saboo
View journal
Vitamin D Deficiency and Its Association with Clinical Parameters in Type 2 Diabetes: Findings From a Cross-Sectional Study in India
Authors: Pramod Tripathi; Nidhi S. Kadam; Thejas Kathrikolly; Diptika Tiwari; Baby Sharma; Anagha R. Vyawahare; Malhar H. Ganla; Mamata Hiremath; Banshi D. Saboo
View journal -
EUROPEAN CONGRESS ON OBESITY (ECO) 2024 | Venice, Italy| 12th - 15th May 2024

Abstract No. GC4.085, Page No. 356
Overcoming Obesity and Type-2-Diabetes in Indian Population: A Holistic Lifestyle Intervention Approach
Authors: Pramod Tripathi, Diptika Tiwari, Nidhi Kadam, Thejas Kathrikolly, Anagha Vyawahare, Baby Sharma, Malhar Ganla, Nikhil Bhanagay, Amrutha Prabhu, Pournima Kulkarni, Bansi Saboo
Note: Please click on the link below to take you to the pdf page of the complete list of abstracts. To locate our abstract please search for the abstract number highlighted above the title. View journalAbstract No. GC4.259, Page No. 444
Effect of a Year-Long Lifestyle Intervention Program on Metabolic Health in Individuals with Obesity in India
Authors: Pramod Tripathi, Anagha Vyawahare, Nidhi Kadam, Malhar Ganla, Thejas Kathrikolly, Diptika Tiwari, Baby Sharma, Nikhil Bhanagay, Bansi Saboo
Note: Please click on the link below to take you to the pdf page of the complete list of abstracts. To locate our abstract please search for the abstract number highlighted above the title. View journal -
International Congress on Integrative Medicine and Health (ICIMH) 2024 | Cleveland OHIO | 9th - 13th April 2024

Abstract No. OA16.02
Effectiveness of a lifestyle intervention program in improving mental health outcomes among adults with type 2 diabetes in India
Authors: Dr. Pramod Tripathi, Ms. Baby Sharma, Dr. Nidhi Kadam, Dr. Pournima Kulkarni, Dr. Diptika Tiwari, Dr. Thejas Kathrikolly, Mrs. Anagha Vyawahare, Dr. Mayurika Biswas
View journalAbstract No. P16.02
Holistic Lifestyle Medicine for Reversal and Remission of Type 2 Diabetes: Insights from an Indian Population Study
Authors: Dr. Pramod Tripathi, Dr. Nidhi Kadam, Dr. Thejas Kathrikolly, Dr. Diptika Tiwari, Mrs. Anagha Vyawahare, Ms. Baby Sharma
View journalAbstract No. P16.03
Positive Health Transformation and Weight Reduction in Obese Patients Following Lifestyle Intervention
Authors: Dr. Pramod Tripathi, Mrs. Anagha Vyawahare, Dr. Nidhi Kadam, Dr. Thejas Kathrikolly, Dr. Diptika Tiwari, Ms. Baby Sharma
View journal -
IDF 2023 | International Diabetes Federation | Virtual | 4th - 7th December 2023

Efficacy of a Lifestyle Intervention program in improving mental health among Patients with Type 2 Diabetes in India
Authors: Ms. Baby Sharma, Dr. Pramod Tripathi, Dr. Nidhi Kadam, Mrs. Anagha Vyawahare, Dr. Diptika Tiwari, Dr. Thejas Kathrikolly, Dr. Mayurika Das Biswas
View journalInsulin resistance and sensitivity in context of dyslipidaemia in non-obese type 2 diabetes patients
Authors: Dr. Diptika Tiwari, Dr. Pramod Tripathi, Dr. Nidhi Kadam, Mrs. Anagha Vyawahare, Ms. Baby Sharma, Dr. Thejas Kathrikolly, Dr. Malhar Ganla, Dr. Banshi Saboo
View journalLifestyle Intervention for Dyslipidemia in Type 2 Diabetes: Insights from an ongoing Diabetes Management Program
Authors: Dr. Thejas Kathrikolly, Dr. Pramod Tripathi, Dr. Nidhi Kadam, Mrs. Anagha Vyawahare, Ms. Baby Sharma, Dr. Diptika Tiwari
View journal -
SICEM 2023 | Seoul International Congress of Endocrinology and Metabolism | Seoul, Republic of Korea | 26th - 28th October 2023

Is Return to a Normal Glycaemic Profile a Possibility in Patients with Type 2 Diabetes Undergoing Remission through a Lifestyle Intervention Program?
Authors: Dr. Pramod Tripathi, Dr. Nidhi Kadam, Dr. Diptika Tiwari, Mrs. Anagha Vyawahare, Ms. Baby Sharma, Dr. Thejas Kathrikolly, Dr. Malhar GanlaComorbidities and glycemic control challenges in type 2 diabetes: a baseline profile of patients attending a diabetes management program
Authors: Dr. Nidhi Kadam, Dr. Pramod Tripathi, Dr. Thejas Kathrikolly, Dr. Diptika Tiwari, Mrs. Anagha Vyawahare, Ms. Baby Sharma, Dr. Malhar GanlaWeight loss-induced type 2 diabetes remission in the non-obese Indian population through a customized lifestyle intervention program
Authors: Dr. Pramod Tripathi, Mrs. Anagha Vyawahare, Dr. Nidhi Kadam, Dr. Diptika Tiwari, Ms. Baby Sharma, Dr. Thejas Kathrikolly, Dr. Malhar GanlaSubgroups of Type 2 Diabetes and their Association with Weight Loss-induced Remission through Lifestyle Intervention in Indian Population
Authors: Dr. Pramod Tripathi, Mrs. Anagha Vyawahare, Dr. Nidhi Kadam, Dr. Diptika Tiwari, Ms. Baby Sharma, Dr. Thejas Kathrikolly, Dr. Malhar Ganla -
EASD Hamburg 2023 | European Association for the Study of Diabetes | Hamburg, Germany | 2-6th October 2023

Possibility of Clearing Oral Glucose Tolerance Test in Type 2 Diabetes Patients Who Underwent Complete Diabetes Remission
Background/objective: Type 2 diabetes (T2D) remission through calorie and carbohydrate restriction has been reported. We conducted a pilot trial to observe whether oral Glucose tolerance test (OGTT) clearance is possible in T2D patients who underwent remission through a lifestyle modification program.
Methods: A total of 3689 patients who had previously undergone remission through our one-year lifestyle modification program in Pune city, India, were asked to enroll for the OGTT; 1121 (all still in remission) accepted the invitation and enrolled (June 2022). Remission was defined as HbA1c<48mmol /mol for a minimum of three months without glucose-lowering medication. Of 1121, 400 participants completed a 3-month training (where foods with increasing glycemic load were introduced every week while monitoring the blood sugar levels (BSL)). Subsequently, they appeared for OGTT (75g) from October-November 2022.
Results Of the 400 participants, 207 (51.7%) cleared OGTT [Fasting BSL(FBSL)<=100, 2-hrs postprandial (PP2) <140], 175 (43.7%) cleared IGT-Impaired Glucose Tolerance (FBSL<126, PP2<200), while 18 (4.5%) did not clear. The median BMI at the time of appearing for OGTT was 22.8 kg/m2. Those clearing OGTT had significantly higher weight loss during the program than those clearing IGT (10 kg vs 6.4 kg) and had a shorter duration of diabetes (5 years vs 6.9 years) (p<0.05). Medication status at the start of the intervention (OHA, Insulin, both, and no medication) did not affect the possibility of clearing OGTT (p>0.1).
Conclusion Complete remission of type 2 diabetes to the point of achieving a non-diabetes glycemic profile irrespective of initial medication status is possible through lifestyle intervention if weight loss is achieved and maintained. The long-term sustainability of lifestyle interventions in achieving remission needs to be explored through a larger cohort study with a control group.
-
ADA San Diego 2023 | American Diabetes Association | San Diego (CA), USA | 23rd-26th June 2023

- Effectiveness of an Intensive Lifestyle Modification Program on Type 2 Diabetes Remission in Indian Population
- Subphenotyping of Type 2 Diabetes Based on Pathophysiology and Its Association with Diabetes Remission in Urban Indians
- Characteristics of Diabetes Remission in Patients with Type 2 Diabetes
- Improvement in Anxiety and Depression in Patients with Type 2 Diabetes through Customized Lifestyle Intervention
- Possibility of Oral Glucose Tolerance Test Clearance in Patients with Type 2 Diabetes Who Underwent Complete Diabetes Remission
-
IDF Lisbon 2022 | International Diabetes Federation | Lisbon, Portugal | 5-8th December 2022

Indian scenario of Diabetes Remission: Interim results of an ongoing cohort study on Type 2 Diabetes remission
Background: Type 2 diabetes (T2DM) remission is widely reported across the world. However, there are no large-scale cohort studies, especially in Indian population.
Aim: To evaluate the effectiveness of a structured community-based lifestyle modification program- ‘Freedom from diabetes holistic transformation program (FFD-HTP) on T2DM remission in Indian population.
Materials and methods: Patients with diagnosed T2DM (HbA1C > 6.5 or on conventional diabetes medication) above 18 years of age were included in a one-year intense lifestyle modification program, ‘FFD-HTP’. The intervention includes dietary modifications (high protein, low carbohydrate vegan diet, with low glycemic fruits and vegetables), personalized exercise plan (anti-gravity, yoga poses, cardio workout), and stress management support (psychological counselling, mindfulness meditation), with regular monitoring through a personal mentor. HbA1C and other biochemical parameters were measured at baseline, every three months, and after completion of the study, while fasting and post prandial blood glucose levels were measured daily. Complete T2DM remission was defined as maintaining HbA1c<6.5 for at least 3 months without use of anti-diabetic medication.
Results: A total of 3,103 patients were screened between December 2020 and March 2021. Of these, 1,127 (699 males) met the inclusion criteria. Mean age was 51.7±10.4 years with mean duration of diabetes 10.4±7.6 years. After one-year intervention, 416 patients (36.9%) achieved T2DM remission. Patients were divided into four groups: Groups A (on oral hypoglycemic agents [OHA], n=829), B (on both insulin and OHA, n=219), C (only on insulin, n=4), and D (not on any anti-diabetic medication, n=75), respectively. In group A 41.7% (n=346) patients, group B 5.9% (n=13) patients, and group D 76% (n=57) patients achieved complete remission, with no remission in group C.
Conclusion: Our findings tentatively suggest that FFD-HTP is beneficial in achieving T2DM remission in Indian population. A one-year post-intervention follow-up is underway to understand the long-term effects of the intervention.
-
PSAD-RAPID Copenhagen 2022 | PsychoSocial Aspects of Diabetes' Annual Scientific Meeting | Copenhagen, Denmark | 29th November- 1st December 2022

Impact of Intensive Lifestyle Intervention On Depression And Anxiety In Patients With Type 2 Diabetes – A Way Forward
Background: Type 2 diabetes (T2DM) is a chronic metabolic disorder that has a significant impact on mental health of an individual. In turn, depression and anxiety result in poor disease outcome and early mortality in patients with T2DM.
Objective: The study aimed to assess the effect of holistic lifestyle intervention in improving depression and anxiety in patients with T2DM.
Materials and Methods: In this quasi-experimental study, baseline data on 250 T2DM patients enrolled in a one-year online holistic lifestyle intervention programme at the Freedom from Diabetes Clinic (Pune, India) between May-August 2021 was collected. Data on anthropometric parameters and medical history was collected along with response to validated Patient Health Questionnaire (PHQ-9) (scoring 0-27) and Generalized Anxiety Disorder Assessment (GAD-7) scale (scoring 0-21). The intervention comprised of customized vegan diet and exercise protocol along with following activities to improve mental health: meditation, diary writing, goal setting, and one-on-one psychological counselling sessions. At the completion of 6 months of intervention, the patients were re-administered the questionnaires to see the effect in improving the PHQ-9 and GAD-7 scores. Since the intervention is for one year, data collection is ongoing.
Results: At baseline, the prevalence of depression and anxiety (score>10) was 13% and 15% which reduced to 9.3% and 8.9% post-intervention, respectively. Post intervention, depression (3.30+4.35) and anxiety scores (3.27+4.21) were statistically lower than baseline (4.28+4.49 & 4.59+5.16) (Z= -3.73; -4.25, p<0.05) , respectively (using Wilcoxon signed rank test). Of the 32 patients with depression and 38 patients with anxiety at baseline, those who regularly attended the inner transformation phase and one-on-one psychological counselling session /s, 10 showed an improvement in depression scores and 20 showed improvement in anxiety scores.
Conclusion: Our findings suggest that incorporating a psychological component to lifestyle interventions may help improve mental health in patients with T2DM.
NATIONAL
-
ISLM | International Conference on Lifestyle Medicine | Chennai, India | 31st Oct – 2nd November 2025

Psychological Burden in Indian Type 2 Diabetes Patients: The Prevalence, Overlap, and Predictors of Diabetes Distress, Depression, And Anxiety
Kiran Vaswani, Baby Sharma, Pramod Tripathi, Nidhi Kadam, Anagha Vyawahare, Diptika Tiwari, Thejas Kathrikolly, Malhar Ganla, Banshi Saboo -
RSSDI 2025 | Research Society of the Study of Diabetes in India | Kochi, Kerela, India | 6th - 9th November 2025

1] Impact of Intensive Lifestyle Intervention on Atherogenic Lipid Profile and Cardiovascular Risk Estimation in Indian Adults with Obesity
Authors: Diptika Tiwari, Pramod Tripathi, Nidhi Kadam, Anagha Vyawahare, Baby Sharma, Thejas Kathrikolly, Amruta Prabhu, Malhar Ganla, Banshi Saboo
2] Beyond Glycemic Control: Assessing Mental Health Comorbidities in Indian Adults with Type 2 Diabetes
Authors: Baby Sharma, Pramod Tripathi, Nidhi Kadam, Diptika Tiwari, Thejas Kathrikolly, Anagha Vyawahare, Amruta Prabhu, Malhar Ganla, Banshi Saboo
3] Impact of Structured Lifestyle Intervention on Body Composition and Diabetes Remission in Obese Indian Women with Type 2 Diabetes
Authors: Anagha Vyawahare, Pramod Tripathi, Nidhi Kadam, Diptika Tiwari, Baby Sharma, Thejas Kathrikolly, Malhar Ganla, Amruta Prabhu, Banshi Saboo
4] Intensive Lifestyle Intervention Improves Glycemic Control and Reduces Medication Dependence in Individuals with Long- standing T2D on Glucose-lowering Therapies
Authors: Thejas Kathrikolly, Pramod Tripathi, Nidhi Kadam, Anagha Vyawahare, Baby Sharma, Diptika Tiwari, Amruta Prabhu, Malhar Ganla, Banshi Saboo -
56th Nutrition Society of India -Annual National Conference | Pune, India | 14th & 15th November 2024

Positive Impact of a One-Year Online Lifestyle Intervention On Glycemic Control, Dyslipidemia, Hypertension, And Remission Rate In Severely Obese T2D Patients
Authors: Tanmayi Naik, Pramod Tripathi, Anagha Vyawahare, Nidhi Kadam
-
Scientific Session on Diabetes & Obesity Metamorphosis | Pune, India | 30th June 2024

Holistic Health Management: Comprehensive Lifestyle Approaches to Manage Obesity and Type 2 Diabetes in India
Authors: Aparna Mudholkar, Pramod Tripathi, Diptika Tiwari, Nidhi Kadam, Baby Sharma, Thejas Kathrikolly, Anagha Vyawahare, Malhar Ganla
-
SYM-HEALTH 2024 (National Conference on Sustainable Healthcare Systems for Population and Planet Health) | Pune, India | April 26th – 27th 2024

Optimising Health: A Comprehensive Lifestyle Intervention Approach in Overcoming Obesity and Type-2-Diabetes in Indian Population
Authors: Mrs. Tanmayi Naik Pathak, Dr. Pramod Tripathi, Dr. Diptika Tiwari, Dr. Nidhi Kadam
-
Chellaram Diabetes Institute - 8th International Diabetes Summit-2024 | Pune, India | 15th – 17th March

Sub-classification of type 2 diabetes in drug-naïve patients: Assessing remission rates across identified clusters
Authors: Dr. Pramod Tripathi, Dr. Amruta Prabhu, Mrs. Anagha Vyawahare, Dr. Nidhi Kadam, Dr. Malhar Ganla, Dr. Thejas Kathrikolly, Dr. Diptika Tiwari, Ms. Baby Sharma, Dr. Banshi Saboo
Effects of intensive lifestyle intervention on lipid and metabolic profiles in patients in type 2 diabetes remission: A comparison of normal and impaired glucose tolerance groups
Authors: Dr. Pramod Tripathi, Dr. Diptika Tiwari, Dr. Nidhi Kadam, Dr. Amruta Prabhu, Dr. Banshi Saboo
Integrated intensive lifestyle intervention improves cardiovascular risk factors in patients with type-2 diabetes
Authors: Dr. Pramod Tripathi, Dr. Thejas Kathrikolly, Dr. Nidhi Kadam, Dr. Amruta Prabhu, Dr. Banshi Saboo
Diabetes and mental health: A cross-sectional study on prevalence and determinants of diabetes distress, depression, and anxiety in type 2 diabetes patients in India
Authors: Dr. Pramod Tripathi, Ms. Baby Sharma, Dr. Nidhi Kadam, DR. Amruta Prabhu -
DIABETES INDIA 2024 | 14th World Congress Of Diabetes India | Bhubaneswar, Odisha | 25th - 28th, January, 2024

1. Holistic Lifestyle Intervention for Prediabetes Management: A Year-long Study on Weight Loss, Glycaemic Control, and Lipid Improvements in an Indian Population
Authors: Dr. Diptika Tiwari, Dr. Pramod Tripathi, Dr. Nidhi Kadam, Dr. Banshi Saboo
2. Exploring Lifestyle Modification for Dyslipidemia Management in Type-2 Diabetes: Early Insights from an Ongoing Diabetes Reversal Program in India.
Authors: Dr. Pramod Tripathi, Dr. Thejas Kathrikolly, Dr. Nidhi Kadam, Mrs. Anagha Vyawahare, Ms. Baby Sharma, Dr. Diptika Tiwari, Dr. Banshi Saboo -
Vishwa Swasthyam ICIGH (International Conference on Integrative Global Health) | Mumbai, India | 4th – 6th January 2024

Holistic Lifestyle Intervention In Prediabetes Management And Restoring Wellness
Authors: Mrs. Tanmayi Naik, Dr. Pramod Tripathi, Dr. Diptika Tiwari, Mrs. Anagha Vyawahare, Ms. Baby Sharma, Dr. Thejas Kathrikolly, Dr. Malhar Ganla, Dr. Nidhi Kadam -
RSSDI 2023 | Research Society of the Study of Diabetes in India | Mumbai, India | 16th - 19th November 2023

P21: Enhancing Type 2 Diabetes Classification Strategies: Data-Driven Comparative Insights from Cluster Analysis and Sub-Phenotyping
Authors: Mrs. Anagha Vyawahare, Dr. Pramod Tripathi, Dr. Nidhi Kadam, Dr. Diptika Tiwari, Ms. Baby Sharma, Dr. Thejas Kathrikolly, Dr. Malhar GanlaP22: Prevalence and Predictors of Anxiety and Depression among Individuals with Type 2 Diabetes in India
Authors: Ms. Baby Sharma, Dr. Pramod Tripathi, Dr. Nidhi Kadam, Mrs. Anagha Vyawahare, Dr. Diptika Tiwari, Dr. Thejas Kathrikolly, Dr. Mayurika Das BiswasP83: Impact of lifestyle intervention on glycemic control and remission in type 2 diabetes patients with normal BMI
Authors: Dr. Pramod Tripathi, Dr. Nidhi Kadam, Dr. Amruta Prabhu, Mrs. Anagha Vyawahare, Dr. Thejas Kathrikolly, Ms. Baby Sharma, Dr. Diptika Tiwari, Dr. Malhar GanlaTo read our abstracts, click here
-
ISLM | International Conference on Lifestyle Medicine | Chennai, India | 4th - 5th November 2023

Impact of Lifestyle Medicine on Type 2 Diabetes Remission in Indian population
Authors: Dr.Pramod Tripathi, Dr.Nidhi Kadam, Dr Kiran Vaswani, Dr.Thejas Kathrikolly -
NAMSCON Bengaluru | 63rd Annual Conference of the National Academy of Medical Sciences | Bengaluru, India | 6th-8th October 2023

Holistic Tele-Counselling combined with visual feedback through a smartphone application to improve self-management in Type 2 Diabetes Mellitus patients between the age group of 40-79 years
-
DiaCareCon Ahmedabad | Annual Conference of DiaCare | Ahmedabad, India | 30th September-1st October 2023

1. Interplay between ABC Goals, Insulin Resistance Indices, Beta-Cell Function, and Dyslipidemia in Patients with Type 2 Diabetes
Background: The ABC goals (HbA1c <7%, blood pressure < 140/90 mmHg, and LDL-C <100 mg/dl) serve as crucial benchmarks for the management of type 2 diabetes (T2D) as well as associated comorbidities.
Objective: The study aimed to explore the interrelationship between ABC goals, insulin resistance (IR), beta-cell function (BCF), and dyslipidemia in T2D patients.
Method: We retrospectively analysed the baseline data of clinically diagnosed T2D patients (not on Insulin) attending a one-year online lifestyle intervention programme for diabetes management at the Freedom from Diabetes Clinic, India. The data included medical history, anthropometric, and biochemical parameters. Homeostasis model assessments of insulin resistance (HOMA-IR), beta-cell function (HOMA-β), and quantitative insulin-sensitivity check index (QUICKI) were calculated.
Results: Data on 681 patients on medications for diabetes, dyslipidemia, and hypertension were analysed. Of the total, 22.3%, 44.9%, and 26.9% of patients achieved all three, two, or one ABC goals, respectively; 5.9% of patients did not achieve any of the ABC goals. Patients who met all three goals showed significantly lower insulin resistance, higher sensitivity (HOMA-IR, median 2.1; QUICKI, median 0.34), higher BCF (median 62.9), and healthier lipid profiles than those who did not achieve all three goals (p<0.05). Patients achieving only two goals showed significantly healthier lipid profiles (p<0.05) compared to those who either met a single goal or did not meet any goal. A significantly higher number of elderly patients achieved ABC goals compared to those below 50 years of age (p<0.05). No significant association was observed between diabetes duration and ABC goal achievement (p>0.1).
Conclusion: Achieving the ABC goals may be challenging for T2D patients due to IR and altered BCF. Further research to explore this relationship may aid in effective diabetes management and better patient outcomes.
2. Lifestyle Intervention for Promoting Weight Loss, Diabetes Management, and Remission in Obese Type-2- Diabetes Patients
Background: Obesity and type 2 diabetes (T2D) pose a multifaceted public health challenge. Lifestyle intervention to achieve diabetes remission among obese T2D patients is an area of ongoing investigation.
Objective: This study aimed to investigate the effectiveness of a comprehensive lifestyle intervention program in promoting weight loss, diabetes management and remission among obese patients with T2D.
Methods: Data were collected on obese (BMI>30 kg/m2) T2D-diagnosed patients (>18 years) (n=470) enrolled in a one-year lifestyle modification program at Freedom from Diabetes Clinic, Pune between April to December 2021. The intervention included a plant-based diet, physical activity, psychological support, and medical management. Baseline and endline anthropometric and biochemical parameters (lipid profiles and glycemic indices) were analyzed. Remission was defined as maintaining HbA1c < 6.5% for a minimum of 3 months without the use of anti-diabetic medication.
Results: Post-intervention, a significant reduction in body weight (91 kgs to 84 kgs, p<0.05) and improvement in glycemic control (HbA1c reduced from 7.7% to 6.6%, p < 0.05) were observed. Further, 50% of patients showed significant improvement in BMI; 46% shifted to the overweight category (BMI 25-30 kg/m2) while 4% shifted to the normal BMI category (BMI<25 kg/m2). Additionally, 37% of the population achieved remission with higher rates of remission (46%) associated with more than 5 kgs weight loss (p<0.05). Furthermore, significant improvements in triglycerides and HOMA-IR values (p<0.05) were also observed.
Conclusions: Significant improvement in weight loss and glycemic control observed in the study underscores the efficacy of a comprehensive lifestyle intervention in facilitating remission in obese individuals with T2D. These findings emphasize the importance of lifestyle modifications as a reliable approach for the effective management of T2D among obese individuals.
-
IDEC Pune 2023 | International Diabetes Experts Consortium | Pune, India | 30th June- 2nd July 2023

Possibility of Oral Glucose Tolerance Test (OGTT) Clearance in Type 2 Diabetes Patients who underwent Complete Diabetes Remission
Improvement In Anxiety and Depression in Patients With Type 2 Diabetes Through Customized Lifestyle Intervention
-
D-TechCon New Delhi 2023 | World Congress of Diabetes Technology & Therapeutics | New Delhi, India | 5-7th May 2023

Prevalence and Determinants of Anxiety and Depression in Patients with Type 2 Diabetes in India
-
Diabetes India Indore 2023 | Diabetes India | Indore, India | 5-7th April 2023

1. Characteristics of Type 2 Diabetes Remission in Non-Obese Indian Population
Background & Aim: Weight loss-induced Type 2 Diabetes (T2D) remission is widely reported in overweight and obese but not in those with normal BMI. Indians are known to have higher body fat at normal BMI. The study aimed to evaluate the effectiveness of a one-year lifestyle modification program on weight-loss-induced T2D remission in non-obese Indian population.
Materials and methods: We retrospectively analyzed data on anthropometric and biochemical parameters of T2D patients (with prior informed consent) with normal BMI (18.5 to 25 kg/m2) enrolled in an online one-year diabetes management program. The intervention included a customized plant-based diet, exercises, stress management, and medical support. Remission was defined as HbA1c<48 mmol /mol for a minimum of 3 months without the use of anti-diabetic medications.
Results: The mean age, duration of diabetes, and BMI at baseline were 41.8±12 years, 10.6±11.9 years, and 22.8±2.3 kg/m2, respectively (n=515). Post-intervention, mean weight, fasting blood glucose, fasting insulin, and HbA1c decreased significantly (p<0.05). Remission was seen in 69 (13.3%) patients. Higher remission was seen in those with>5% weight loss and diabetes duration <6 years (36.2%) followed by those with <5% weight loss and <6 years of diabetes duration (26.8%). Those with >6 years of diabetes duration showed lower remission irrespective of the weight loss.
Conclusion: Our findings suggest that patients with normal BMI with recently diagnosed T2D can also achieve remission through lifestyle management with a weight loss of at least 5%. However, the rate of remission is lower in patients with normal BMI compared to that reported in overweight and obese patients in previous studies in the Indian population.
2. Sustained Type 2 Diabetes Remission through Lifestyle Modification in a Geriatric Patient: A case report with 3-year follow-up
Background: The common factors influencing Type 2 diabetes (T2D) remission include the recent diagnosis, lower age, and minimal dosage of medicines. The current case study reports sustained T2D remission post-one-year lifestyle intervention program in an elderly male on a high dose of insulin.
Case presentation: An elderly male patient (60 years) with obesity (BMI 31.7 kg/m2) and diagnosed with T2D (3.4 years back) enrolled for a one-year lifestyle intervention program at our diabetes management clinic. At the first consult, he was on 94 units of insulin and oral hypoglycemic agents with an HbA1c of 8.7%. Other significant history included microalbuminuria (106 µg/ml). The intervention included a customized plant-based diet, exercises, stress management, and medical support. At the end of the program, he had a weight loss of 13 kg, stopped both insulin and OHAs, showed significant improvement in HbA1c (4.9% without medication) and urine microalbumin (3.2 µg/ml), and successfully cleared the 75g oral glucose tolerance test (OGTT). He continues to be in remission and has cleared the OGTT for 3 consecutive years.
Conclusion: We present three unique features in the current case report: (1) The elderly age of the patient and high insulin dosage, (2) OGTT clearance along with normalization of HbA1c, and (3) reversal of associated co-morbidity. The current case study shows that despite older age and higher dosage of insulin, the patient achieved complete T2D remission through sustained weight loss by following our lifestyle modification program. Future experimental studies with adequate sample sizes would help substantiate our observation.
3. A Case Report on Remission of Long-Standing Type 2 Diabetes through Lifestyle Modification in a Geriatric Patient
Background: Weight loss through lifestyle modifications is known to induce Type 2 diabetes (T2D) remission; however, in recently diagnosed younger populations. Here we report the complete remission (defined as maintaining HbA1c <6.5% for at least three months without the use of diabetes medication) in an elderly patient with a 30-year history of T2D, through customized lifestyle modification.
Case Presentation: In December 2019, a 66-year-old male patient diagnosed with T2D (HbA1c 7.7%) and on both insulin and oral hypoglycemic agents (OHA) presented to our clinic. Other medical history included hypertension, hyperlipidemia, and multiple surgeries. Family history revealed that the patient’s mother had T2D. He enrolled in our one-year lifestyle modification program which included a customized plant-based diet, exercises, stress management, and medical management support. The patient underwent complete remission with a reduction in HbA1C (5.3%), fasting insulin (8.62 μU/ml), fasting blood sugar (85mg/dl), postprandial blood sugar (104mg/dl), and homeostatic model assessment of insulin resistance (HOMA-IR) (6.22 to 1.81) at the end of the program. He also successfully cleared the 75g oral glucose tolerance test (OGTT). The patient continues to be in remission based on his last follow-up visit in May 2022 (HbA1C 5.3%). Informed consent was obtained from the patient for reporting the case study.
Conclusion: We present three unique features in the current case report: 1) The patient’s advanced age, 2) longer duration of diabetes, and 3) HbA1c normalization with OGTT clearance. Younger age and lower diabetes duration are common positive predictors of T2D remission documented in earlier studies. The current case study shows that despite older age and longer T2D duration, it is possible to undergo complete remission along with OGTT clearance through lifestyle modification. Future planned studies with adequate sample sizes would help substantiate our findings.
4. Prevalence and Determinants of Anxiety and Depression in Patients with Type 2 Diabetes in India
Background & Aim: Type 2 diabetes (T2D) is a chronic metabolic disorder that has a significant impact on the mental health of an individual, which in turn results in increased morbidity and mortality. Aim of the present study was to assess the prevalence of anxiety and depression and its determinants in patients with T2D attending a diabetes management clinic in India.
Materials and Methods: Patients enrolling for a one-year online diabetes management program in India between July 2021 and September 2022 were invited to participate in this cross-sectional study. Data on medical history, anthropometry, and biochemical parameters were collected. The validated Patient Health Questionnaire (PHQ-9) (scoring 0-27) and Generalized Anxiety Disorder Assessment (GAD-7) scale (scoring 0-21) were used to assess depression and anxiety, respectively. Statistical analyses were performed using SPSS 21. P-value<0.05 was considered statistically significant.
Results: A total of 2730 (34.5% females) patients with T2D agreed to participate (gave informed consent) and completed the questionnaires. The mean age and duration of diabetes were 49.9±10.2 and 10.0±7.0 years, respectively. The prevalence of moderate to severe depression and anxiety was 20.3% and 17.3%, respectively. Both depression and anxiety were significantly higher in females, those who were overweight and obese, those who were less than 50 years of age, had recently been diagnosed (<6 years), those with poor glycemic control (HbA1c> 8%), and those on insulin (p<0.05). Conclusion: Gender, higher BMI, lower age, recent diagnosis, use of insulin, and poor glycemic control were factors affecting both anxiety and depression in T2D patients in India. The high prevalence of both depression and anxiety suggests the inclusion of psychological aspects in the management of T2D in the Indian population.
-
RSSDI Chennai 2022 | Research Society of the Study of Diabetes in India | Chennai, India | 6-9th October 2022

Effectiveness of a customized lifestyle modification program on Type II Diabetes Remission: Indian Scenario
-
FEMPEDICON, Nashik | Indian Academy of Pediatrics | Nashik, India | 30-31st July 2022

Effectiveness of a structured community-based lifestyle modification on Remission of Type II Diabetes: Indian Scenario
YEAR-WISE DOCUMENTATION OF GTT CLEARED PARTICIPANTS
Glucose Tolerance Test (GTT) involves consuming 15 tsp (75 grams) of glucose in a fasting state. This is followed by checking Blood Sugar Level (BSL) tests, taken after one and two hours respectively. Only those whose BSL counts fall within normal ranges are declared successful. All diabetics usually fail this test. Infact, this test is used to diagnose diabetes and pre-diabetes. Many medical professionals consider it to be one of the ultimate test of reversal.
Over the years the number of FFD participants who have successfully cleared this test has grown tremendously, after becoming free of medications and coming into remission (Hba1c < 6.5 without medications for 3 months).
In 2015, we had around 15 GTT cleared participants; By 2021 that number had blossomed to 350+. So far, over 600+ participants have cleared GTT and 400+ have cleared IGT. Conventional thinking may maintain that diabetes is irreversible, but we know this is not true through this real-world experience. It’s a great achievement for anyone who has suffered from diabetes, to stop medications, to experience remission and then clear this tough test and it definitely is a cause of celebration. Summary of the year-wise results are given in the graph below:
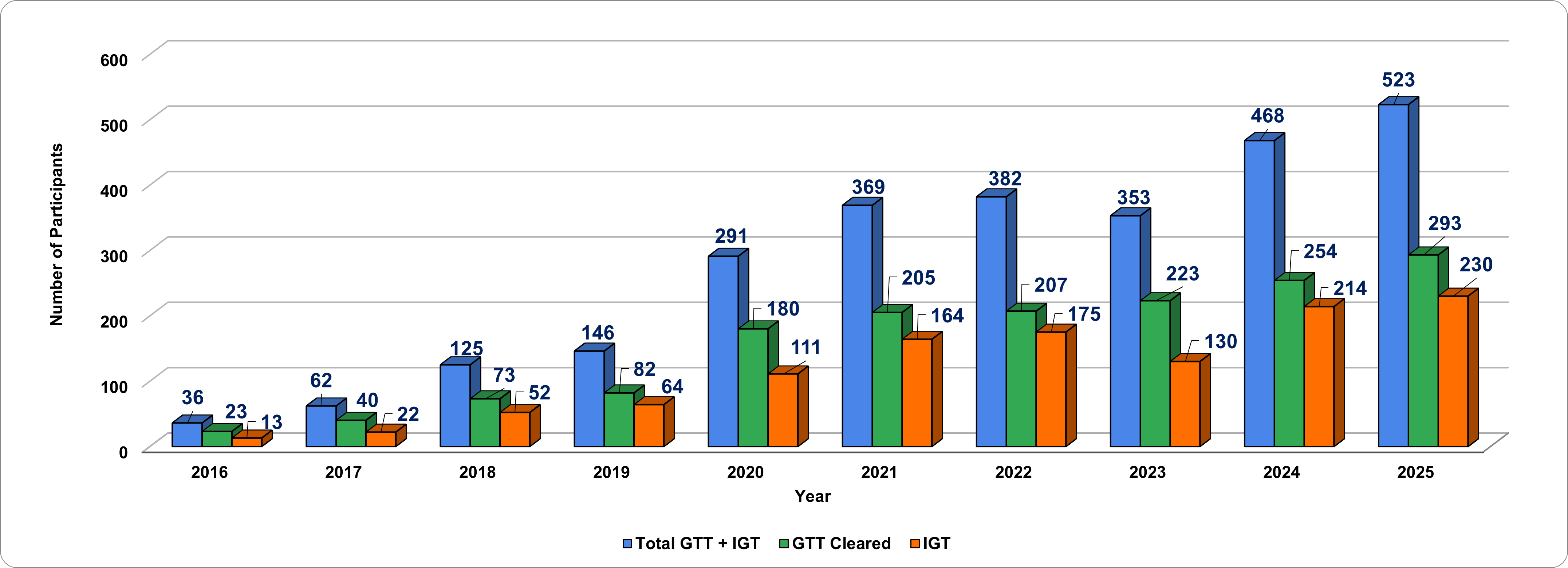
Every year since 2015, we have been celebrating this achievement of our participants through a unique Festival of Freedom called Muktotsav. This is an annual event when our champions step into the well-deserved limelight. They are felicitated and awarded for their achievements. Not just those who have reversed their diabetes, and passed the GTT, but other champions too. For instance, people who have lost the maximum weight, or stopped their medicine in the shortest time. There are also award categories for freedom from hypertension, cholesterol medications, most deserving athletes, healthy couples and families, etc. The successes of our participants validate our efforts and our belief that Diabetes Can Be Reversed. This event greatly encourages other diabetics, from all over the world, to strive towards their own reversal and freedom!
Muktotsav has attracted several celebrity guests. In 2020, Muktotsav had internationally celebrated diabetes reversal pioneer, Dr. Neal Barnard as Chief Guest. In 2021, acclaimed researcher in the field of diabetes remission, Dr. Roy Taylor graced the event as the Chief guest along with Dr. Bhushan Patwardhan (Former Vice Chairman- UGC and Chairman- Indian Council of Social Science Research).
To know more about the people who have achieved this stupendous success, the celebrations and awards, please click on the year wise links below:
- Muktostav 2016 - 36 Participants cleared GTT/IGT
- Muktostav 2017 - 62 Participants cleared GTT/IGT
- Muktostav 2018 - 125 Participants cleared GTT/IGT
- Muktostav 2019 - 146 Participants cleared GTT/IGT
- Muktostav 2020 - 291 Participants cleared GTT/IGT
- Muktostav 2021 - 368 Participants cleared GTT/IGT
- Muktostav 2022 - 382 Participants cleared GTT/IGT
- Muktostav 2023 - 351 Participants cleared GTT/IGT
- Muktostav 2024 - 465 Participants cleared GTT/IGT
- Muktostav 2025 - 523 Participants cleared GTT/IGT
